Flexible Cystoscopy Q&A
Cystoscopy is examination of the urethra (waterpipe) and lining of the bladder using a telescope called a cystoscope.
The cystoscope is slightly smaller than the diameter of a ballpoint pen and it is passed up the urethra into the bladder. There are two types of cystoscopes – flexible and rigid.
It is arranged by your urologist and is carried out as an outpatient procedure by the urology nurse specialists.
A flexible cystoscopy is usually performed to discover the cause of blood in the urine (haematuria), causes of bladder irritation, to diagnosis a urethral stricture (narrowing) or to remove a J-J Stent.
A rigid cystoscopy is the same examination of the urethra and bladder using a slightly bigger scope.
This is usually performed under general or spinal anaesthetic.
After the groin area has been cleaned with an antiseptic solution, a local anaesthetic gel is inserted into the urethra.
This stings slightly when it goes in and then the anaesthetic begins to take affect.
The procedure takes approximately 5-10 minutes to perform. Once the local anaesthetic gel has been inserted, the cystoscope is passed up the urethra and into the bladder.
Using a camera attached to the scope, the urethra and bladder are checked for strictures (narrowing), stones, bladder tumours or any other abnormalities. If necessary, small biopsies can be taken down the telescope.
If any further procedures are necessary, this will be discussed with you after the flexible cystoscopy.
If further investigations or surgery are required, a date for rigid cystoscopy under general anaesthetic will be booked.
Flexible cystoscopy is an outpatient procedure carried out in the clinic. At the end of the procedure you will be able to leave the clinic and drive home.
You may experience some minor discomfort or occasional bleeding when passing urine
This usually settles within a day or so. You will be advised to increase your fluid intake up to 2 litres per day for the following two days.
If you develop a temperature or symptoms of cystitis, you may have a urinary tract infection requiring a course of antibiotics.
If this occurs, you should contact either the urology department or your GP for advice.
Cystistat Bladder Therapy Q&A
Cystistat is sodium hyaluronate which is a naturally occurring substance that mimics the bladder’s natural barrier against irritants and infections.
Cystistat assists in repairing the internal bladder wall if it has been damaged or inflamed as a result of disease processes. Over a number of treatments, it allows the bladder’s natural defences to recover, thereby, breaking the inflammation/damage cycle that occurs in these conditions.
Cystistat is used when the integrity of the bladder wall is compromised giving rise to symptoms of pain, urinary frequency and urgency. Disease conditions that can damage the bladder wall include:
- Bladder Pain Syndrome – this condition is of unknown origin and its extreme form is known as Interstitial Cystitis (IC). It results in a chronic inflammation and degeneration of the bladder wall and is usually resistant to antibiotic therapy.
- Recurrent urinary tract infections (UTI) – infections present with the symptoms above and also can include blood in the urine. Bacteria can damage the lining of the bladder wall and this can initiate a cycle of inflammation/damage/further infection, which prevents the bladder being able to repair its defences adequately before a further infection takes hold.
- Radiation-induced Cystitis – radiation therapy can lead to severe cystitis with blood in the urine (haematuria) which can debilitate patients leading to hospitalisation in some cases.
Cystistat is given as bladder instillation therapy. The patient attends as an outpatient and is asked to lie on an examination couch. A small catheter in inserted in the urethral opening and 50mls of the prepared Cystistat treatment fluid is introduced into the bladder. The catheter is then removed and the patient can go home. The patient will be able to drive home without any specific restrictions.
The Cystistat coats the internal surface of the bladder and begins the repair process of the internal wall.
This treatment requires an schedule of interval bladder instillations for maximum benefit. There are a number of schedules available and at Essex Urology we use the following:
- Once weekly for 6 weeks
- Once a fortnight for 3 months
- Once a month for 6 months
We initially tried to change from weekly to monthly treatments and found that patients found that the change was too drastic in terms of symptom control and we compromised with the fortnightly step-down before moving to monthly
Sodium hyaluronate is a naturally occurring substance which is very well tolerated by patients. To date, we have not had any issues with allergy or side effects.
There are no major complications with this treatment. It is sometimes uncomfortable to give the instillation as the urethral opening may be too small for passage of the catheter. If this is the case, your specialist may address this after consultation with a different approach to your management before instillations can continue.
Your progress will be monitored throughout the Cystistat treatment to ensure that improvement in symptom relief is occurring. Assuming that all is well, you may be able to continue monthly Cystistat therapy on a longer term basis.
At Essex Urology, we use Patient Related Outcome Measures (PROMs) to directly assess the patient’s response to treatment. This type of assessment is an important tool for improving healthcare delivery and offers a patient-centred approach to care at the individual level.
Cystometrogram Q&A
This is a test to assess the function and stability of the bladder.
It is arranged by your urologist and is carried out as an outpatient procedure by the urology nurse specialists.
The CMG test is part of the investigations for an overactive bladder. The patient may be complaining of symptoms including urgency and frequency.
This test is also useful in patients complaining of urinary leakage or incontinence and will assess how the bladder reacts on filling and emptying.
Men with bladder outflow symptoms sometimes undergo CMG before proceeding with any operations on the prostate.
This is because symptoms due to prostatic enlargement can be due to the prostate itself, the bladder or a combination of the two.
A small rectal catheter is inserted into the back passage. This is essential to measure the pressure within the abdominal cavity, outside the bladder.
A second small catheter is inserted into the bladder after applying a local anaesthetic gel to the urethra. This is essential for measuring the pressure within the bladder itself.
Once the catheters are in place they are attached to a special machine and your bladder is gently filled with water via the bladder catheter.
During this phase you will be asked various questions. These questions relate to how the bladder fills, if there is any leakage or bladder spasm, etc.
On completion of the test you will be asked to empty your bladder and the two tubes will then be removed.
No. You may feel some discomfort rather than pain as the anaesthetic gel and tubes are inserted.
This test takes approximately 30-45 minutes to complete. At the end of the test, you will be able to leave the clinic and drive home.
Some medications have to be stopped prior to this test, as they will affect the accuracy of the result.
These include oxybutinin (Ditropan), tolteridine (Detrusitol), solfenacin (Vesicare) and trospium (Regurin). If you are not sure about your medications, please contact the department arranging the test to check, well in advance.
The test will not be performed if you have a urinary tract infection (UTI). You will need to seek advice from your GP or district nurse if you feel that you have an infection. You may be required to have a course of antibiotics.
If you are unable to attend your CMG test appointment due to infection, please inform the urology department organising the test so that rearrangements can be made. See contacts.
You may experience some minor discomfort when passing urine for a few days.
This should settle after 48 hours or so. You will be asked to increase your fluid intake to 2-3 litres per day during this time.
At the end of the test, a follow-up appointment will be arranged to discuss the results of the CMG with your specialist. Any medications that were stopped before the test, can be resumed after the CMG has been completed.
Template Guided Prostate Biopsy Q&A
TGBP stands for “Template Guided Biopsy of Prostate” and is also known as Transperineal Biopsy of Prostate or TBP .
Biopsy means taking some very small samples from the prostate so that these may be examined under the microscope to exclude cancer.
Your urologist arranges this test after consultation.
You may be asked to see a urologist in the first instance for a number of reasons, such as urinary symptoms (slow flow, urinary dribbling, getting up at night, etc.) or after having your PSA tested as part of a medical screening.
The Template biopsy is usually indicated for the following reasons to exclude cancer of the prostate:
- Raised PSA blood test
- An abnormal feeling prostate when examined by your urologist
- A combination of the above
TGBP is carried out as a day case procedure under a short general anaesthetic (GA). The patient is given a bowel preparation prior to the procedure to clear the back passage. Antibiotics are given at the time of procedure to reduce the risks of infection.
An ultrasound probe is inserted into the back passage (rectum) and the prostate scan pictures are taken.
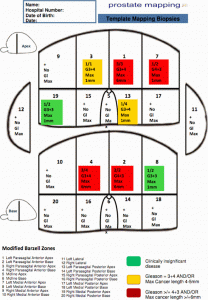
A biopsy needle is then inserted into the skin between the back of the scrotum and the back passage to take samples from the prostate using ultrasound imaging. The surgeon uses a special grid to standardise the biopsy procedure.
Each sample is a thread of prostate tissue, which is collected and sent to the pathology laboratory for examination under the microscope.
Once the sampling is complete, you will be able to leave hospital. You may experience some discomfort for a few days until everything settles down.
You should not drive on the day of the prostate biopsy. The prostate sample analysis may take up to 2 weeks. Mr Thilagarajah’s secretary will contact you as soon as the results are ready.
An appointment will be arranged for you to be reviewed in the outpatient clinic. Depending on the results, further tests and scans may be necessary. This will be discussed with you fully at the consultation.
Common side effects include:
- Blood in the urine – this can occur in the majority of cases. Drink plenty of water and this should settle after about 10 days
- Blood in the semen – this occurs in most patients and you may find that the semen fluid is stained a red colour after this procedure. This may take many weeks to settle and is not of concern. The red colour becomes a brown stain before it disappears
- Perineal bruising – this can occur in up to 20-50% of patients
- Pain or discomfort – can occur in up to 40% of patients
Complications include the following:
- Urine infection – This can occur in a small number of patients (1%). It is important to take the antibiotics given prior to and after the procedure to prevent this happening.
- Erectile problems – usually short-lived and occurs in up to 5% of cases
- Acute retention – in up to 5% of cases and may require temporary catheterisation
- Septicaemia (blood infection) – 1 in 1000 (0.1%) and may require emergency admission to hospital for treatment
Each area can be given a risk category to show how important the cancer in that area might be. These are colour coded to make it easier to visualise the areas that are important.